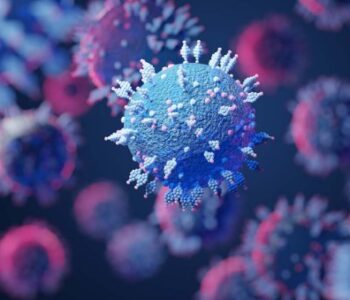
Covid 19 Pandemic
Covid 19 Pandemic
Covid 19 Symptoms And Signs
COVID-19 Symptoms Vary, Ranging From Moderate Symptoms to Severe Sickness.
Headache, loss of smell and taste, nasal congestion and runny nose, cough, muscular discomfort, sore throat, fever, diarrhea, and breathing problems are all common symptoms. People with the same virus may have a variety of symptoms, which may vary over time. A respiratory symptom cluster with cough, sputum, shortness of breath, and fever; a musculoskeletal symptom cluster with muscle and joint pain, headache, and exhaustion; and a digestive symptom cluster with stomach discomfort, vomiting, and diarrhea have all been discovered.COVID-19 is linked to loss of taste and smell in persons who have never had ear, nose, or throat problems, and it has been documented in as many as 88 percent of instances.

Only 81 percent of those who display symptoms have mild to moderate symptoms (up to mild pneumonia), whereas 14 percent develop severe symptoms (dyspnea, hypoxia, or more than 50% lung involvement on imaging), and 5% develop critical symptoms (respiratory failure, shock, or multiorgan dysfunction).
At least a third of those who are infected with the virus never show any signs or symptoms. Asymptomatic carriers are less likely to get tested and hence transmit the illness. Other infected persons may develop symptoms later, referred to as “pre-symptomatic,” or have extremely weak symptoms, and can transfer the virus to others.
There is a lag between when a person gets sick and when the first symptoms occur, as is usual with infections. COVID-19 has a four to five day median delay. Symptoms appear in the majority of sick persons two to seven days after exposure, and virtually everyone has at least one symptom by 12 days.
The majority of patients recover from the disease’s acute phase. However, some individuals – more than half of a cohort of home-isolated young adults – continue to suffer a variety of consequences, including as weariness, for months after recovery, a condition known as chronic COVID; long-term organ damage has also been documented. Long-term research are being conducted to learn more about the disease’s long-term impact.
Transmission
COVID-19 Transmission is the main article.
The pulmonary route of COVID-19 transmission, which includes bigger droplets and aerosols.
When individuals inhale droplets and minute airborne particles (that create an aerosol) that infected persons exhale while they breathe, speak, cough, sneeze, or sing, the illness is mostly spread via the respiratory route.
When infected persons are physically near, they are more likely to transfer COVID-19. Infection may, however, spread across greater distances, especially indoors.

Infectivity might appear 1-3 days before symptoms appear.
Even if they are asymptomatic or pre-symptomatic, infected people may transmit the illness.
In most cases, the peak viral load in upper respiratory tract samples comes close to the beginning of symptoms and then diminishes after the first week. According to current research, viral shedding and infectiousness may last up to 10 days after symptom start in people with mild to moderate COVID-19, and up to 20 days in those with severe COVID-19, including immunocompromised people.
Infectious particles vary in size from small aerosols that float in the air for a long time to bigger droplets that float or fall to the ground.
Furthermore, COVID-19 research has reshaped our knowledge of how respiratory viruses are spread. The biggest droplets of respiratory fluid do not go far and may infect mucous membranes of the eyes, nose, and mouth if breathed or landed on them. When individuals are physically near, aerosols are at their peak concentration, making viral transmission simpler. However, airborne transmission may occur over longer distances, especially in poorly ventilated areas; tiny particles can stay suspended in the air for minutes to hours in certain situations.
Only 10 to 20% of persons are responsible for the disease’s propagation, therefore the number of people affected by a single sick person fluctuates.
It spreads in clusters, with infections linked to an index case or a specific geographic place. In many of these cases, superspreading episodes occur, in which a single individual infects a large number of others.
Coronavirus 2 causes severe acute respiratory syndrome (SARS).
SARSCoV2 is a virus that belongs to the coronavirus family of viruses.
It has a single linear RNA segment and is a positive-sense single-stranded RNA (+ssRNA) virus. Humans, other mammals, including cattle and companion animals, and avian species are all infected by coronaviruses. Human coronaviruses may cause illnesses ranging from the common cold to more serious infections like Middle East respiratory syndrome (MERS, which has a 34% death rate). After 229E, NL63, OC43, HKU1, MERS-CoV, and the original SARS-CoV, SARS-CoV-2 is the sixth known coronavirus to infect humans.
Data on viral genomic sequences may reveal if viruses that are isolated in time and location are likely to be epidemiologically connected.
It is feasible to recreate a phylogenetic tree of a virus family’s mutation history with a sufficient number of sequenced genomes. Five genomes of SARSCoV2 had been identified from Wuhan and reported by the Chinese Center for Disease Control and Prevention (CCDC) and other institutes by 12 January 2020; by 30 January 2020, the number of genomes had climbed to 42. The samples were found to be “strongly linked with at most seven alterations relative to a common ancestor” in a phylogenetic study, hinting that the first human infection happened around November or December 2019. At the outset of the pandemic, the structure of the phylogenetic tree revealed strong similarities between human isolates. As of August 21, 2021, 3,422 SARSCoV2 genomes from 19 strains have been publicly released from all continents except Antarctica.
COVID-19 testing for further details
A nasopharyngeal swab is shown for COVID-19 testing.
Nucleic acid assays, which identify the presence of viral RNA fragments, are the main techniques of testing for the presence of SARS-CoV-2.
The usefulness of these tests to assess the length of infectivity of patients is restricted since they detect RNA but not infectious virus. The test is usually performed on respiratory samples acquired using a nasopharyngeal swab, although it may also be performed on a nasal swab or a sputum sample. The results are usually ready in a matter of hours. The World Health Organization (WHO) has released various illness testing procedures.

CT scans of the chest may be useful in diagnosing COVID-19 in people who have a strong clinical suspicion of infection, but they are not suggested for regular screening.
Early infection is characterized by bilateral multilobar ground-glass opacities with a peripheral, asymmetric, and posterior distribution. As the illness advances, subpleural dominance, crazy paving (lobular septal thickening with varying alveolar filling), and consolidation may emerge. Asymmetric peripheral ground-glass opacities without pleural effusions are common imaging findings on chest radiographs and computed tomography (CT) of persons who are symptomatic.
Prevention
Additional information is available at: COVID-19 pandemic prevention, COVID-19 pandemic face masks, and COVID-19 pandemic social distancing methods. Pathogens may spread rapidly without pandemic containment measures like social separation, immunization, and face masks. This graph depicts how early implementation of containment measures protects a larger portion of the population.

Getting vaccinated, staying at home, wearing a mask in public, avoiding crowded places, keeping a safe distance from others, ventilating indoor spaces, managing potential exposure durations,washing hands with soap and water frequently and for at least twenty seconds, practicing good respiratory hygiene, and avoiding touching the eyes, nose, or mouth with unwashed hands are all preventive measures to reduce the risk of infection.
The CDC advises those who have been diagnosed with COVID-19 or suspect they may be infected to stay at home except for medical care, call ahead before visiting a healthcare provider, wear a face mask before entering the healthcare provider’s office and when in any room or vehicle with another person, cover coughs and sneezes with tissues, wash hands frequently with soap and water, and avoid sharing personal household items.
Vaccines
COVID-19 vaccine is the main topic of this essay.
See also COVID-19 Vaccine Development History and COVID-19 Vaccine Deployment.
A COVID19 vaccine is a vaccine designed to confer acquired immunity against the virus that causes coronavirus illness 2019 (COVID19), the severe acute respiratory syndrome coronavirus 2 (SARSCoV2). Prior to the COVID19 pandemic, there was a well-established body of information regarding the structure and function of coronaviruses that cause illnesses like SARS and Middle East respiratory syndrome (MERS). The development of multiple vaccine platforms was hastened as a result of this information in early 2020.
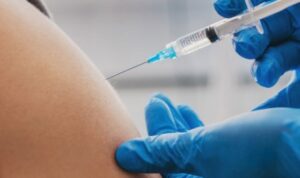
SARS-CoV-2 vaccinations were developed with the goal of avoiding symptomatic, frequently severe sickness. SARS-CoV-2 genetic sequence data was exchanged via GISAID on January 10, 2020, and the global pharmaceutical sector declared a strong commitment to address COVID19 on March 19, 2020. The COVID19 vaccinations have been extensively credited with lowering the severity and fatality rates associated with COVID19.
Many nations have devised staggered distribution programs that prioritize people who are most at risk of difficulties, such as the elderly, as well as those who are most at risk of exposure and transmission, such as healthcare personnel.
The European Union authorized the Pfizer BioNTech vaccine on December 21, 2020. On December 27, 2020, vaccinations started to be delivered. The Moderna vaccine received approval on January 6, 2021, while the AstraZeneca vaccine received approval on January 29, 2021.
On February 4, 2020, US Secretary of Health and Human Services Alex Azar issued a notice of declaration under the Public Readiness and Emergency Preparedness Act for medical countermeasures against COVID-19, stating that the declaration covers “any vaccine, used to treat, diagnose, cure, prevent, or mitigate COVID-19, or the transmission of SARS-CoV-2 or a virus mutating therefrom,” and that the declaration precludes “liability claims alleging negligence by a manufacturer in creating a
[156] According to a research published on the 8th of December, the AstraZeneca vaccine is roughly 70% effective. [157]
More than 4.6 billion doses of COVID-19 vaccination has been delivered in over 190 countries as of mid-August 2021. The vaccination developed by Oxford-AstraZeneca was the most commonly utilized. [158]
Treatment
COVID-19 treatment and management is the main article.
COVID-19 does not have a particular, effective therapy or cure.
[160] Supportive care, which includes treatment to ease symptoms, fluid therapy, oxygen support, and prone posture if required, as well as drugs or devices to assist other afflicted essential organs, is the cornerstone of COVID-19 management. [161]
Invasive ventilation is being given to a severely unwell patient at the intensive care unit of the University of So Paulo’s Heart Institute. A bridge ventilator is being utilized to automatically trigger a bag valve mask due to a scarcity of mechanical ventilators.
The majority of COVID-19 instances are minor. To treat symptoms (fever,[162] body pains, cough), supportive therapy involves medicines such as paracetamol or NSAIDs, as well as enough oral fluid intake and relaxation. [160] [163] A balanced diet and good personal cleanliness are also encouraged. [164] Those who are unwell should remain at home, according to the CDC. [165]
Severe instances may need hospitalization. The glucocorticoid dexamethasone is indicated for patients with low oxygen levels because it may minimize the risk of mortality. [166] To maintain breathing, noninvasive ventilation and, eventually, admission to an intensive care unit for mechanical ventilation may be necessary. [167] To treat respiratory failure, extracorporeal membrane oxygenation (ECMO) has been employed. [168] [169]
Clinical studies are now underway for a number of investigational medicines.
[159] Others that have been deemed to be successful, such as hydroxychloroquine and lopinavir/ritonavir, as well as so-called early therapy, are not advised by US or European health officials. [159] [170] [171] In high-risk situations, two monoclonal antibody-based treatments are available for early usage. [171] The antiviral remdesivir is available with varying restrictions in the United States, Canada, Australia, and a few other countries; however, it is not recommended for use with mechanical ventilation, and the World Health Organization (WHO) discourages its use altogether due to limited evidence of its efficacy. [159]
Variants
SARS-CoV-2 Variants (Main article)
WHO has designated some variations as variants of concern (VoC) or variants of interest (VoI) (VoI). They both had the D614G mutation, which is more contagious: [17
Prognosis
COVID-19 has a range of severity. The illness may have a moderate course with little or no symptoms, similar to other upper respiratory infections like the common cold. Symptoms are severe enough to need hospitalization in 3–4 percent of patients (7.4% for those over 65). [177] Mild instances usually recover in two weeks, whereas severe or critical illnesses might take three to six weeks to recover from. The interval between the beginning of symptoms and death has varied from two to eight weeks in individuals who have died.

[178] The median duration between the beginning of symptoms and death was twelve days, according to the Italian IstitutoSuperiore di Sanità, with seven people being hospitalized. People admitted to an ICU, on the other hand, spent an average of 10 days in the hospital before dying. [179] On arrival to the hospital, a prolonged prothrombin time and high C-reactive protein levels are linked to a severe course of COVID-19 and a transfer to the ICU. [180] [181]
Strategies
COVID-19 Public Health Mitigation is the main article.
Many governments tried to restrict or halt the spread of COVID-19 by advocating, requiring, or forbidding behavioural modifications, while others largely concentrated on delivering information. The measures varied from public warnings to complete lockdowns. Containment and mitigation are two strategies for controlling an epidemic. They may be pursued in any order or at the same time. [182]
Delaying and decreasing the peak strain on healthcare (flattening the curve) as well as reducing total instances and health effect are among the mitigating goals.
[184] Furthermore, boosting healthcare capacity (raising the line) over time, such as by increasing bed count, employees, and equipment, helps to fulfill rising demand. [185]
Masks (like as those worn by Taiwanese President Tsai Ing-wen) are recommended by the CDC and WHO to help prevent the transmission of SARS-CoV-2.
Containment
Containment is the process of preventing an epidemic from spreading to the wider public. Individuals that are infected are isolated while they are contagious. People they’ve come into touch with are contacted and isolated for long enough to confirm they’re not sick or infectious. Rt is reduced to less than 1 after successful containment or suppression. [186]

Screening is the first step in the containment process. Screening involves looking for symptoms in order to identify sick people who may subsequently be isolated and/or treated. [187]
Mitigation
If containment fails, efforts will shift to mitigation, which involves taking steps to prevent the spread of the virus and reduce its impact on the healthcare system and society.
The term “flattening the epidemic curve” refers to the process of delaying and reducing the peak of an epidemic.
[183] This reduces the danger of overburdening health-care systems and gives researchers more time to create vaccinations and therapies. [183]
Interventions that aren’t pharmacological
Personal actions such as hand hygiene, wearing face masks, and self-quarantine; community measures aimed at reducing interpersonal contacts such as closing workplaces and schools and canceling mass gathering events; community engagement to encourage acceptance and participation in such interventions; and environmental measures such as surface cleaning are all non-pharmaceutical interventions that may help manage the outbreak.
[188] Many of these steps have been criticized as hygiene theater, such as scrubbing surfaces. [189]
Additional measures
Attempts have been made in several jurisdictions to take more harsh measures, such as quarantining whole communities and imposing stringent travel limits.
[190] The most severe restrictions have been imposed by China and Australia. The most stringent travel restrictions were imposed by New Zealand. South Korea used widespread screening and localized quarantines, as well as issuing notifications about infected people’s travels. Singapore gave financial assistance, isolated those who did not comply, and fined those who did not. Taiwan expanded face mask manufacture and penalized medical supply hoarding. [191]
Tracing of contacts
See also: COVID-19 pandemic mitigation software use and development and COVID-19 pandemic mitigation public health information technology.
Contact tracing is a method of trying to discover recent contacts of newly infected people in order to test them for infection.
[192] Traditionally, infectees are asked to provide a list of contacts, which are subsequently contacted by phone or in person.
Another method is to gather location data from mobile devices in order to identify persons who have had considerable interaction with infectees, albeit this has raised privacy issues.
[193] Google and Apple unveiled a privacy-preserving contact tracking endeavor on April 10, 2020. [194] [195] Palantir Technologies first supplied COVID-19 tracking services in Europe and the United States. [196]
Health-care services
Additional information: Flattening the curve, a list of nations organized by hospital beds, and COVID-19 pandemic shortages
In Brazil, there is a makeshift hospital for COVID-19 patients.
The WHO describes increasing capacity and tailoring healthcare to the requirements of COVID-19 patients as a crucial outbreak response strategy.
[197] The ECDC and the WHO’s European Regional Office issued guidelines for hospitals and primary healthcare services to shift resources at multiple levels, such as focusing laboratory services on COVID-19 testing, canceling elective procedures, separating and isolating COVID-19 patients, and increasing intensive care capabilities by training personnel and adding ventilators and beds. [197] [198] Telehealth has exploded as a result of the epidemic. [199]
Manufacturing on the fly
Some manufacturers have begun 3D printing nasal swabs and ventilator components due to capacity constraints in conventional supply chains.
[201] For example, after reverse-engineering and printing one hundred required ventilator valves overnight, an Italian startup got legal threats for suspected patent infringement.
[202] NASA claimed creating a ventilator in 37 days on April 23, 2020, which is now being tested. [203] [204] Individuals and groups of makers generated and shared open source ideas, as well as gadgets that were made using locally found materials, sewing, and 3D printing. Face shields, protective robes, and masks in the millions were produced. Shoe coverings, surgical caps, motorized air-purifying respirators, and hand sanitizer were among the other improvised medical equipment. Ear savers, non-invasive ventilation helmets, and ventilator splitters are examples of novel equipment. [205]
Immunity of the herd
Several specialists raised worry in July 2021 that obtaining herd immunity may not be attainable at this time since the Delta variation is transferred among persons who have received existing immunizations.

[206] The CDC released data demonstrating that persons who had been vaccinated may transmit the Delta form, something experts thought was impossible with other versions. As a result, the WHO and the CDC recommend those who have been vaccinated to continue taking precautions including social distance and wearing masks inside. [207]
History
COVID-19 pandemic timeline (main article)
Additional information: Pandemic prevention and forecasts, as well as preparations for the COVID-19 pandemic
2019 In this essay, we’ll look at the timeline for the COVID-19 pandemic in 2019.
Aerial image of the market, which seems to be under development.
After being shut down, the Huanan Seafood Wholesale Market reopened in March 2020.
Desc-i.svg
Confirmed instances per million persons are shown on an interactive timeline map.
(may not work on mobile devices; drag circle to adjust)
The epidemic was detected in Wuhan in November 2019, despite the fact that the virus’s specific origin is still unclear. Many early instances of COVID-19 were connected to visitors to Wuhan’s Huanan Seafood Wholesale Market, although it’s probable that human-to-human transmission occurred before then. [26] [27] According to a retrospective investigation, the number of COVID-19 cases in Hubei rapidly climbed beginning in December 2019, reaching 60 by December 20 and at least 266 by December 31. [208]
A bronchoalveolar lavage fluid (BAL) sample from an unresolved clinical case was delivered to sequencing firm Vision Medicals on December 24, 2019.
[209] The findings of the test were reported to the Wuhan Central Hospital and the China CDC (CCDC) on the 27th and 28th of December, indicating the presence of a new coronavirus. [209] [210] On the 26th of December, a pneumonia cluster of unknown origin was discovered and treated by Doctor Zhang Jixian at Hubei Provincial Hospital. On December 27, he notified the Wuhan Jianghan CDC. [211]
On December 30, 2019, a test report from business CapitalBioMedlab mailed to Wuhan Central Hospital showed an erroneous positive result for SARS, prompting Wuhan Central Hospital physicians to notify their colleagues and hospital officials. Eight of those physicians were eventually warned by the police for spreading false rumors, including Li Wenliang (who was also penalized on 3 January)[212], while another doctor, Ai Fen, was reprimanded by her supervisors. [213] The Wuhan Municipal Health Commission (WMHC) issued an alert to medical institutes that evening about “the treatment of pneumonia of unknown etiology.” [214] The following day, WMHC issued the first public disclosure of an unidentified cause pneumonia epidemic, confirming 27 cases[215][216][217]—enough to warrant an inquiry. [218]
The WHO office in China was notified on December 31st of instances of pneumonia with an unknown etiology in Wuhan.
[215] At the beginning of January 2020, an investigation was begun. [218]
Early occurrences, according to official Chinese sources, were largely related to the Huanan Seafood Wholesale Market, which also sold live animals.
[220] CCDC director George Gao said in May 2020 that animal samples gathered from the market had tested negative, suggesting that the market was not the cause of the first epidemic. [221] WHO released its assessment in March 2021, saying that transmission via an animal host was the most plausible scenario, while bats and the food supply chain were not ruled out. [2] [25]
2020 COVID-19 pandemic
COVID-19 pandemic timelines by month for 2020: January, February, March, April, May, June, July, August, September, October, November, and December
On March 20, 2020, Chinese physicians in Huanggang, Hubei.
Chinese officials reported 44 instances of “pneumonia of unknown etiology” to WHO between December 31, 2019 and January 3, 2020.

[222] The Chinese National Health Commission informed WHO on 11 January that the epidemic was linked to market exposures and that China had discovered a new strain of coronavirus, which it had isolated on 7 January. [219]
In the beginning, the number of cases doubled every seven and a half days.
[223] The virus expanded to other Chinese regions in early and mid-January, aided by the Chinese New Year migration. Wuhan operated as a significant rail junction and transportation center. [224] The virus’ genome was provided through GISAID on January 10th. [225] According to a retrospective research published in March, 6,174 persons had reported symptoms by January 20th,[226], with the possibility that more had been affected. [227] Given the virus’ “pandemic potential,” a study released on January 24 suggested human transmission, urged personal protective equipment for health professionals, and encouraged testing. [39] [228] The first published modeling research, released on January 31, predicted “independent self-sustaining epidemics in major cities throughout the world” and urged for “large-scale public health measures.” [229]
On the 30th of January, WHO declared the epidemic a Public Health Emergency of International Concern, citing 7,818 illnesses (PHEIC).
[230][231] WHO labeled it a pandemic on March 11th. [232][233]
Italy got its first confirmed illnesses on the 31st of January, in two Chinese visitors.
[234] Italy surpassed China as the nation with the most recorded fatalities on March 19. [235] The United States has surpassed China and Italy as the nation with the most confirmed illnesses by March 26. [236] According to genomic sequencing, the bulk of confirmed illnesses in New York originated from Europe rather than Asia. [237] Prior samples indicated a person infected on December 27, 2019[238][239] in France, and a person in the United States who died from the sickness on February 6, 2019. [240]
In the absence of artificial ventilation, a patient in Ukraine in May 2020 wears a diving mask.
In October, the WHO claimed that one out of every 10 people on the planet, or 780 million individuals, may have been infected, with just 35 million illnesses verified.
Pfizer revealed trial data for a potential vaccine on November 9th, indicating 90 percent efficacy against severe illness.
[242] Novavax submitted an FDA Fast Track application for its vaccine on that day. [243]
Public Health England said on December 14 that a variation has been detected in the UK’s southeast, mostly in Kent. Variant of Concern 202012/01 exhibited alterations to the spike protein that might make it more infectious. A total of 1,108 illnesses has been confirmed as of December 13th. [244]
2021 COVID-19 pandemic
COVID-19 pandemic timelines in 2021, organized by month: January, February, March, April, May, June, July, August, September, October, November, and December
VOC-202012/01, a form of SARS-CoV-2 initially detected in the United Kingdom, was discovered in 33 nations on January 2nd.
The P.1 variety was originally discovered in Japanese travelers returning from Brazil on January 6th.
A WHO-led team of scientists arrived in China on 14 January to investigate the virus’s origins and track out intermediate hosts between the initial reservoir and humans.

In a clinical experiment in South Africa on January 29, it was shown that the Novavax vaccine was only 49% effective against the 501.V2 strain.
[249] In a clinical experiment in Brazil, the China COVID-19 vaccine CoronaVac was shown to be 50.4 percent effective. [250]
Due to blood clotting issues, notably cerebral venous sinus thrombosis, various nations discontinued using the Oxford-AstraZeneca COVID-19 vaccination on March 12th (CVST).
[251] The WHO and the European Medicines Agency found no relation to thrombus on March 20, prompting some nations to restart vaccination. [252]
India was the first place where the Delta variety was discovered. The variety was initially discovered in the UK in mid-April, and two months later it had spread to a third wave, causing the authorities to postpone the planned reopening from lockdown in June. [253]